Shin Splints or Medial Tibial Stress Syndrome (MTSS) is a common injury that affects runners of all ages and levels. Lets take a closer look at how you can recognise and best manage MTSS:
Diagnosis
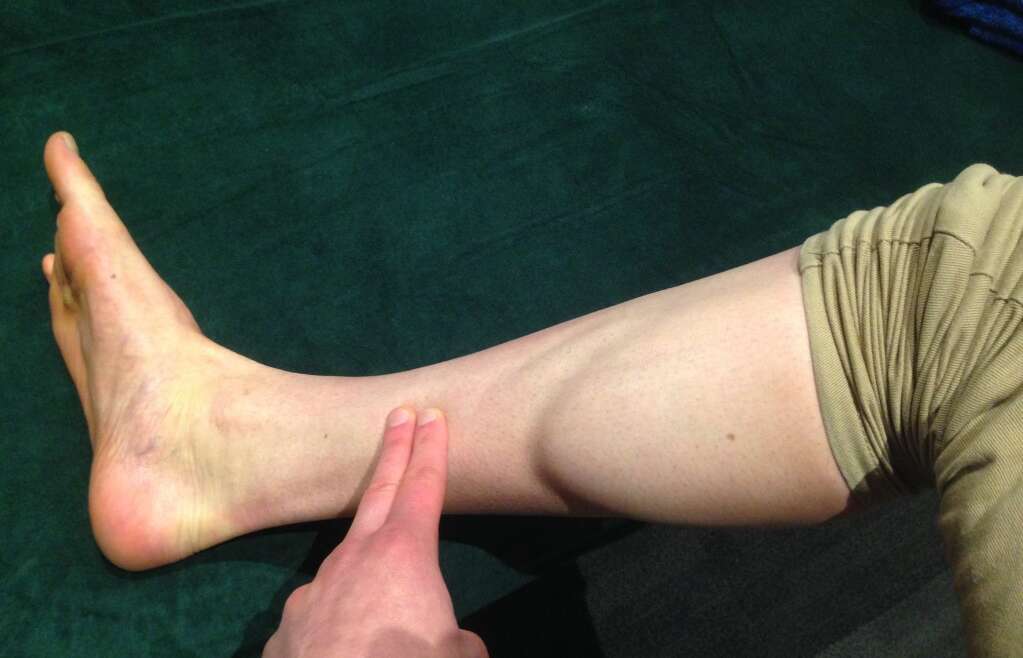
• This is an injury located at the lower end of the shin bone and behind the inside border of the tibia bone
• Stress fractures account for 16% of injuries experienced by runners(1), 23% of these stress fractures occur in the tibia (shin bone)(2)
• Early recognition and accurate diagnosis is key: History, recognition of site of pain and biomechanical overload, imaging helps stage severity and return to sport
• Runners present with pain and tenderness to touch the medial (inside) shaft of the tibia, this becomes worse with exercise.
• MRI is best diagnostic tool, allowing concurrent bony and soft tissue evaluation, MRI can also stage medial tibial stress syndrome(3). Bone scans (scintigraphy) are also highly sensitive however associated radiation exposure is a disadvantage.
Fredericson MRI classification for tibial stress fractures(4):
| Grade 1: periosteal edema only Grade 2: bone marrow edema visible on T2-weighted images Grade 3: bone marrow edema visible on T1- & T2-weighted images Grade 4: intracortical signal abnormalities |
• Most stress fractures heal within 8 weeks through conservative treatment (exercise alteration, exercise rehabilitation, and manual therapy)
• Avoid nonsteroidal anti-inflammatory drugs (NASIDs) such as Nurofen (ibuprofen) and Voltaren (diclofenac), these delay bone healing.
Rehabilitation
| Phase 1 | Phase 2 (2 weeks after walking pain free) |
| • Rest of the area • Maintain aerobic fitness • Manual therapy • Light local strength training of the effected area |
• Whole body muscular endurance training 2-3 times per week eg. sets of 25 calf raises • Gait analysis and retraining • Core/pelvic control • Balance/proprioception • Flexibility |
• Return to running beginning at 30-50% of the pre-injury distance at reduced intensity. This should not increase by more than 10% in distance or pace each week.
• Successful rehabilitation and prevention of recurrence:
| Risk factor | Detection | Management |
| Biomechanical overload | Gait analysis | Running retraining, strength training |
| Training overload | Training history | Implement training plan |
• Avoiding hills early on in recovery reduces risk of incurring stress fractures.
• Including periods of cross training or water running helps avoid tissue overload in return to running.
• Nutrition is important when healing stress factures and requires adequate calcium and vitamin D.
Rehabilitation Targets
Dorsi Flexion Decelerating Muscles:
Soleus – bent knee calf raises, 2 legs, the 1 leg, increased weight, increased speed into hopping
Gastrocnemius – straight knee calf raises 2 legs, 1 leg, hopping
Foot strengthening: – theraband toe flexion, standing raises to ball of foot
Eversion control muscles:
Tibialis posterior – theraband inversion resistance
Gluteus maximus – bridge, hip thrust, Bulgarian split squat, deadlift, overhead rotation lunge
In addition, feel free to check other blogs from our experienced practitioners such as what is the posterior chain which we hope will add a lot of value.
About the Author
Dr. Brendan O’Loughlin is a Co-director and Osteopath at the Competitive Sports Clinic located in the Essendon District, Melbourne Brendan has a keen interest in sports injuries, exercise rehabilitation and cycling and analysis.
References
1. Chen YT, Tenforde AS, Fredericson M. Update on stress fractures in female athletes: epidemiology, treatment, and prevention. Curr Rev Musculoskelet Med. 2013;6(2):173–181.
2. McCormick F, Nwachukwu BU, Provencher MT. Stress fractures in runners. Clin Sports Med. 2012;31(2):291–306.
3. Kahanov, L., Eberman, L. E., Games, K. E., & Wasik, M. Diagnosis, treatment, and rehabilitation of stress fractures in the lower extremity in runners. Open acc j sports med. 2015; 6:87-95.
4. Fredericson M, Bergman AG, Hoffman KL, Dillingham MS. Tibial stress reaction in runners. Correlation of clinical symptoms and scintigraphy with a new magnetic resonance imaging grading system. Am J Sports Med. 1995;23(4):472–481.